Pages in this section:
1. Diabetes can be cured: probiotics
2. Curing diabetes using herbs, spices and dietary supplements
3. Curing diabetes: healthy oils
Cure for diabetes discovered
by Mark Hyman, MD Last Updated August 18, 2012
Recently, I attended a convention of the American Diabetes Association in New York City where the main booth heralded a breakthrough "cure" for diabetes. Excited to think I might learn something new, I hustled right over. Imagine my dismay when all the information at the booth was about weight-loss surgery!
Do we need a cure? Absolutely! Is surgery a one-size-fits-all solution for diabetes? No way.
I understand the desire to find a solution. After all, Type 2 diabetes is looming as the biggest epidemic and public health issue in human history. Close to 300 million people are affected worldwide and another 150 million forecast to be diagnosed by 2030. The reason? Obesity. Yes, obesity is a tenacious problem but surgery is only a Band-Aid solution, albeit one that is growing in popularity. In the last decade alone, the rate of weight-loss surgeries performed each year in the United States has increased from 10,000 to 230,000. But how many of the 1.7 billion overweight citizens of the world can afford gastric bypass? And how many of those will regain the weight?
I have seen many patients go under the knife for these procedures only to gain back the weight they lost, plus some. Weight-loss surgery may seem like a panacea, but it won’t solve the underlying hormonal and metabolic imbalances that are driving the diabetes and obesity. My patient Alan is a prime example. Alan has been overweight since he was 6 years old and has never experienced a day without ravenous hunger. At age 40, he had gastric-bypass surgery and shrunk from 450 to 250 pounds. The size of his stomach changed, but his overall lifestyle did not. Eventually, he gained back 100 pounds. Even with a stomach the size of a walnut, he managed to gain weight one tiny, fattening bite at a time. By the time he landed in my office, he was 60 years old and tired of juggling all the complications of weight-loss surgery.
The Reality of Gastric Bypass: What Doctors Don’t Tell You
Alan is hardly an anomaly. A report on the effectiveness of weight-loss surgery published by the Agency for Healthcare Research and Quality found that within 3 to 5 years after laparoscopic gastric banding, as many as one-third of patients are not able to maintain weight loss due to noncompliance with a prescribed diet and other issues. Plus, the complications stemming from lap-band surgery were as high as 30 percent. We also know that weight-loss surgery is not without risks. Altering the gastrointestinal tract can lead to nutritional deficiencies that require lifelong monitoring and supplementation of calcium, vitamin B12, folate, multivitamins, iron, and thiamine. And the psychological risks of these surgeries are often underplayed. In 2010, a study published in the American Journal of Medicine showed a dramatic increase in suicide among patients who had bariatric surgery, most occurring within three years following the surgery.
Even more disturbing is the rise in overweight teens choosing weight-loss surgery. Since the late ‘90s, the number of weight-loss procedures performed on teenagers has skyrocketed. Some studies show the mean age of these young patients is just 16 years old with some as young as 12! Very few studies have looked at the long-term ramifications of these surgeries. What kind of problems are we passing on to our youth?
A Better Solution
Instead of glorifying the ability of weight-loss surgery to stem the tide of Type 2 diabetes in this country, we need to remember that Type 2 diabetes is an entirely preventable and reversible lifestyle disease. Let me repeat, there is clear evidence from the scientific literature that diabetes is reversible, especially if it is caught early and treated aggressively through lifestyle intervention and nutritional support, and occasionally with medications. (4) In many cases even later stage diabetes can be reversed with very intensive lifestyle changes, medications and supplements.
A groundbreaking new study from England showed unequivocally that people with advanced Type 2 diabetes, when the pancreas has lost its oomph and the insulin-producing (beta) cells are damaged, can reverse the course of the disease in just one week by optimizing dietary strategies, such as eating low-glycemic foods and by staying on a low-calorie diet.
One week! The best news is that dietary changes alone can help your body heal. Studies of patients who have weight-loss surgery show that even a dramatic change in diet in a short period of time creates beneficial metabolic changes. (6) All the metrics we thought were related to obesity, such as high blood sugar, high cholesterol, high blood pressure, inflammation, and clotting, are drastically reduced even without significant weight loss due to the rapid effects of dietary changes on the body (for more information on how to reverse diabetes with diet, see The Blood Sugar Solution.)
Let me be clear, maintaining a healthy weight is ideal for optimal health. But we shouldn’t be signing up for surgery without exhausting every other avenue. Curing diabetes with surgery relies on outdated ideas about the origins of disease and overlooks the complex web of biology as well as the social, political, and economic conditions at the root of our current epidemic.
Please stay away from these drugs for type 2 diabetes
Article by Dr. Michael Murray Sunday, October 6th 2013
Introduction
The research is quite clear – oral medications to treat type 2 diabetes do not alter the long-term progression of the disease. While these drugs can be quite effective in the short term, several different types are associated with increased all cause mortality and in particular an increased risk for dying due to cardiovascular disease.
In addition, often the type 2 diabetic fails to make necessary lifestyle and dietary changes to improve/reverse their condition because these drugs also create a false sense of security.
Ultimately all of these drugs lose their effectiveness over time and start a viscous cycle where they are prescribed at higher dosages or in combination with other drugs, all of which leads to an
even greater rate of mortality. In fact, the long-term use of some of these drugs is actually associated with an earlier death compared to control groups with type 2 diabetes not being given the
drugs.
Background Data:
The most widely prescribed drug for type 2 diabetes is metformin (Glucophage). While studies have shown that metformin alone has illustrated a decrease in heart attacks and all diabetes related
deaths compared with other drugs, it does not work at all in about 25 percent of cases and tends to lose its effectiveness with time. When the latter happens it is usually combined with a
sulfonylurea, which actually increases mortality risk. On their own, these sulfonylureas drugs are of limited value and there is some evidence to indicate that sulfonylureas actually produce harmful
long-term side-effects. For example, in a famous study conducted by the University Group Diabetes Program (UDGP), it was shown that the rate of death due to a heart attack or stroke was 2.5 times
greater in the group taking tolbutamide (a sulfonylurea), than the group controlling their type 2 diabetes by diet alone.
Though newer sulfonylureas are promoted as being safer than tolbutamide, new data calls into that widely held belief into question.
Examples of sulfonylureas:
acetohexamide (Dymelor)
chlorpropamide (Diabinese, Insulase)
glimepiride (Amaryl)
glipizide (Glipizide, Glucotrol)
glyburide (Diabeta, Micronase)
repaglinide (Prandin)
Another class of oral diabetes drugs that appear to increase risk of mortality are the thiazolidinediones such as pioglitazone (Actose) and rosglitazone (Avandia). The first drug in this class, Rezulin (troglitazone), was removed from the market because widespread deaths occurred due to liver failure. Now pooled results from 42 different studies with Avandia showed there was a 43 percent increase in the number of heart attacks and a 64 percent increased risk of dying from heart disease compared to people with type 2 diabetes given a placebo. In addition, both Actose and Avandia are also associated with significant weight gain. While these drugs may have some benefits in lowering blood sugar levels, it is clear that the side effects outweigh these benefits.
Diabetes drugs tied to pancreatitis: study
Article by Andrew M. Seaman | Reuters NEW YORK (Reuters Health)
People who take a certain type of diabetes drug to lower blood sugar levels may be at an increased risk of developing an inflamed pancreas, according to a new study.
Glucagonlike peptide 1(GLP-1) therapies that include exenatide - marketed as Byetta by an alliance between Bristol-Myers Squibb and AstraZeneca - and sitagliptin - marketed as Januvia by Merck - have been linked to pancreatitis before in studies on animals and small groups of patients, said the study's lead author. "New therapies and risks are only evaluated when studies are done. We need to know (the drugs) are effective in lowering blood sugar, but we also need to know about risks," said Dr. Sonal Singh, from the Johns Hopkins University School of Medicine in Baltimore.
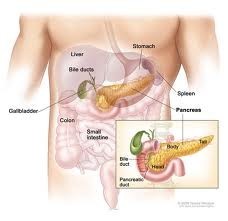
Pancreatitis, which can cause life-threatening complications, is rare but more common in people with type 2 diabetes. Singh said pancreatitis occurs in about three of every 1,000 diabetes patients. The U.S. Centers for Disease Control and Prevention estimates that there are about 19 million Americans diagnosed with diabetes, and another 7 million who have the disease but don't know it yet. In people with type 2 diabetes, the body doesn't produce enough insulin or is resistant to what it does produce.
For the new study, published in JAMA Internal Medicine, the researchers used data on 1,269 diabetes patients between the ages of 18 and 64 years old, who were admitted to U.S. hospitals with pancreatitis in 2005 through 2008. They compared those to 1,269 other diabetes patients who were similar, but were not hospitalized with pancreatitis. Overall, they found 87 of the diabetes patients with pancreatitis were taking GLP-1 therapies, compared to 58 of the diabetes patients without pancreatitis. Singh told Reuters Health that the findings show the drugs are linked to a doubling of the risk of pancreatitis - about six cases per 1,000 diabetics. "I won't say you should be alarmed about the findings, but it's something you should consider," he said. ‘CHANGING TREATMENT'
Dr. Aaron Cypess, a staff endocrinologist in the clinic of the Joslin Diabetes Center in Boston, said the new study will not change how he treats patients, but it may influence him to go over his patients' risk factors for pancreatitis. "For me personally it's not going to change my practice pattern in terms of stopping the drugs, but we may revisit whether you're showing any of the risk factors," said Cypess, who was not involved with the new study.
In a joint statement, the American Diabetes Association and the American Association of Clinical Endocrinologists also said the new findings should not change how doctors treat diabetes patients. "The analysis is a retrospective study using data from an administrative database. This type of analysis is not considered as robust as a prospective randomized controlled clinical trial, the gold standard for evaluating treatments," the organizations wrote in the statement. They continue that there are nine of those "gold standard" trials in the works that should provide answers soon. The current study also had limitations, including that the diabetes patients hospitalized with pancreatitis tended to lead a less healthy lifestyle than those who did not have the condition.
In a commentary, Belinda Gier and Dr. Peter Butler from the University of California, Los Angeles, write supporters say the drugs are safe and offer some advantages over older medications. Currently, the labels for Januvia and Byetta carry warnings that there have been reports of pancreatitis in people taking the drugs. Other side effects of Byetta include nausea and other stomach issues. For Januvia side effects also include respiratory infections and headaches. Cypess told Reuters Health both drugs are still protected by patents and can be expensive. Representatives from Merck and Bristol-Myers Squibb said they - along with drug regulators - actively monitor reports of adverse events in users of their drugs, and have not found evidence showing the drugs cause pancreatitis.
SOURCE: http://bit.ly/YJFiEm JAMA Internal Medicine, online February 25, 2013.
Incurable autoimmune disorders can be treated successfully with functional medicine
Article from natural news by Michelle Goldstein
December 19, 2013
Autoimmune disorders are defined as conditions in which the immune system mistakenly attacks healthy tissue. There are more than 80 types of auto-immune disorders including multiple sclerosis (MS), rheumatoid arthritis, type I diabetes, lupus and inflammatory bowel disease. The American Autoimmune Related Disease Association estimates that 50 million Americans suffer from an autoimmune disorder, with increasing prevalence. Allopathic physicians treat many of these illnesses with powerful immune-suppressing drugs and consider them to be incurable, chronic and often progressive diseases. The goal of their treatment is to suppress symptoms of the diseases, since the underlying causes are considered to be unknown.
To the contrary, innovative holistic health practitioners approach autoimmune disorders as treatable, in which hidden underlying causes are addressed. They also use approaches that improve the
immune system, allowing for remarkable recoveries. Treatments include use of low-dose naltrexone (LDN), reduction of metal toxicity, correcting nutritional deficiencies and addressing underlying
infections. Infections can include parasites, bacteria, viruses and fungi. These approaches share the underlying premise that the immune system has been overloaded with toxins and nutritional
deficiencies, causing an overwhelmed immune system or immune system dysfunction.
Low-dose naltrexone is effective in treating auto-immune disorders
In 1985, Dr. Bernard Bihardi began treating patients who had HIV, cancer and autoimmune disorders with LDN, which is an inexpensive medication that has already been approved for use in higher doses
to treat drug addiction. Bihardi has reported tremendous success in hundreds of patients, including over 400 MS patients. LDN halts autoimmune disorders and other diseases by increasing levels of endorphins produced at night. Endorphins
in turn have been shown to stimulate and improve the immune system. A study reported in 2007 in the American Journal of Gastroenterology and completed at the prestigious Pennsylvania State
University College of Medicine reported LDN therapy to be safe and effective for patients with Crohn's disease. The Journal of AIDS and HIV Research reported an October 2011 study demonstrating the successful use of
LDN in treating HIV/AIDS patients. Other research on LDN effectiveness can be seen here: http://www.lowdosenaltrexone.org.
Treating multiple sclerosis with detoxification and diet
Multiple sclerosis is a serious autoimmune disease that is often progressive and extremely disabling. Ann Boroch, in Healing Multiple Sclerosis, discusses her successful treatment of herself
and hundreds of patients by focusing on dietary changes and treating the hidden infectious cause of the disease, Candida albicans overgrowth. She reports that her dietary program for
eliminating the fungus Candida will also destroy parasites, viruses and bacteria which can promote the disease. Eliminating heavy metals and reducing stress are other essential components of
her recovery program.
The Specific Carbohydrate Diet and GAPS program for inflammatory bowel disease
Elaine Gottschall's Breaking the Vicious Cycle details a dietary program which eliminates grains and certain dairy products in an effort to reverse inflammatory bowel disease. This protocol
has been effective for thousands of individuals. Dr. Natasha Campbell-McBride, author of Gut and Psychology Syndrome, outlines a strong nutrient-dense dietary program based on the Specific
Carbohydrate diet but also includes heavy metal detoxification protocols using juicing.
Conclusions
Conventional medicine treats autoimmune disorders as incurable diseases requiring a lifetime of strong immune-suppressing prescription medications. Alternative practitioners view autoimmune disorders
as an overwhelmed immune system caused by toxicity and nutritional deficiencies. The holistic approaches to many of these "immune system dysfunctions" include increasing the functioning of the immune
system, eliminating infectious agents, decreasing metal toxicity and following a specific nutrient-dense diet which includes targeted nutritional supplements.